The cost-benefit of long-acting injectable buprenorphine as a treatment for opioid use disorder
September 25, 2025 • Reading time 3 minutes
Opioid use disorder (OUD), a chronic and relapsing condition characterised by the compulsive use of opioids, is associated with a wide range of adverse outcomes. Individuals living with OUD experience a range of physical and mental health problems, alongside elevated risks of unemployment, socioeconomic deprivation, homelessness, and contact with the criminal justice system compared to the general population. According to the World Health Organization, opioids account for around 70% of drug-related deaths worldwide. With around 300,000 people affected in England, OUD continues to represent a significant burden on public health.
In recognition of these challenges, the UK government’s From Harm to Hope 10-year drugs strategy (HM Government, 2021) outlines a commitment to rebuilding and expanding treatment services, with the goal of helping an additional 24,000 people achieve long-term recovery. The strategy emphasises the importance of linking recovery to wider socioeconomic outcomes, such as reductions in crime, improvements in sustained employment, and greater access to stable housing, while also aiming to prevent nearly 1,000 drug-related deaths.
Delivering on these ambitions will require not only expanding access to services, but also expanding treatment options to overcome barriers that prevent people from remaining in recovery. Opioid dependence is notoriously difficult to treat; not only because of the complexities of the condition itself, but also due to limited treatment options and obstacles in treatment administration. Although pharmacological options such as methadone and sublingual buprenorphine have proven to be effective, these treatments require daily dosing, which create barriers to entry or lead to adherence challenges for some people.
Long-acting injectable buprenorphine (LAIB) overcomes one key challenge in treating opioid dependence, namely that of daily medication management. Administered once per month by a healthcare professional (with a weekly formulation available to meet individual needs), LAIB has the potential to support longer treatment retention. Edge Health was commissioned by Camurus to evaluate the potential benefits of sustained engagement in treatment with LAIB, alongside its associated costs, in order to assess its overall socioeconomic impact in England as a treatment for OUD.
What we did
To understand the true potential of LAIB, we set out to explore both the scale of opioid use disorder (OUD) in England and the human dynamics that shape it; who enters treatment, who leaves, and who never makes it in. Our approach was firmly rooted in evidence, combining academic literature, cost data, and standard health economic methods to build a robust picture. We examined the wide-ranging costs of OUD under current practices, particularly methadone, and asked how these could shift with the introduction of LAIB. What stood out was LAIB’s unique ability to engage people who might otherwise struggle with the daily demands of traditional treatments, enabling more people to start and remain in recovery. The impacts were quantified by applying the appropriate unit costs, and a benefit-cost ratio (BCR) was calculated.
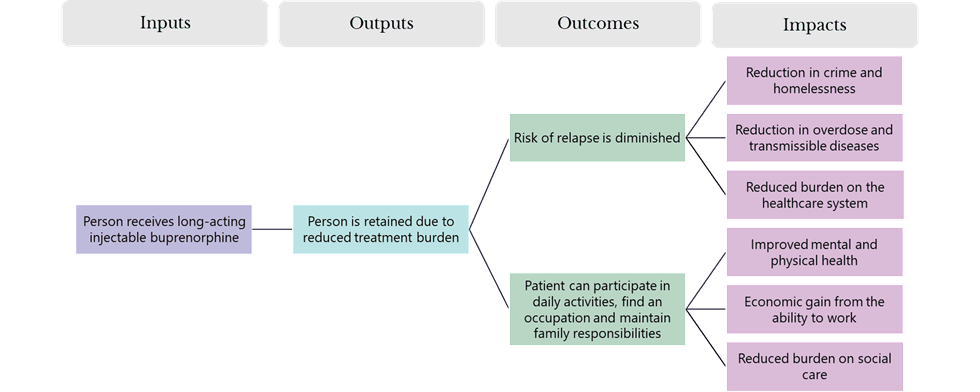
What we found
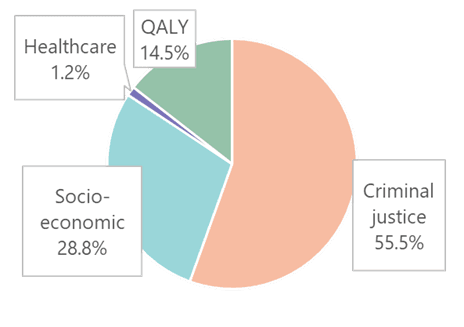
Our evidence review demonstrated that LAIB delivers positive impacts extending beyond clinical outcomes to wider social and economic benefits. We found improvements across employment, reductions in crime and incarceration, lower demand on social care and healthcare services, better quality of life, and the prevention of fatalities. When these outcomes were brought together in the cost-benefit model, the results were highly encouraging: although LAIB involves higher treatment costs, the broader societal benefits substantially outweigh them. Overall, the findings indicate that LAIB is a cost-effective intervention with the potential not only to improve outcomes for people with OUD, but also to deliver considerable value to society. Its wider adoption represents an opportunity to strengthen England’s response to the profound challenges of opioid dependence.
“It has been a pleasure to engage and work with Edge Health on a project to bring to life real-world evidence in a way that is impactful for health policy. The team demonstrate the intellectual curiosity required to rapidly understand an unconventional and potentially complex area of healthcare. Edge brings genuine passion and collaboration to their work. It is a privilege to recommend them to others.”
Daniel Mogford
Camurus Medical Affairs Director UK & Ireland
References
United Nations Office on Drugs and Crime. (2023). World Drug Report 2023. https://www.unodc.org/res/WDR-2023/WDR23_Exsum_fin_DP.pdf
HM Government. (2021). From harm to hope: a 10-year drugs plan to cut crime and save lives. https://assets.publishing.service.gov.uk/media/629078bad3bf7f036fc492d1/From_harm_to_hope_PDF.pdf
 Back to News & Insights
Back to News & Insights
